Get Best Treatment for Glaucoma (Kala-Motia)
- Affordable and best Glaucoma treatment by the top surgeons
- Most advanced treatment of Glaucoma
- Free Online consultation on Glaucoma
"*" indicates required fields
Glaucoma: What Is It?
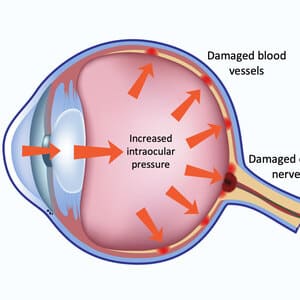
Glaucoma is generally associated with a build-up of pressure inside the eye also called Intraocular Pressure (IOP). This happens when the fluid, aqueous humour inside the eye stops draining from the eye.In Glaucoma, the eye fluid drainage system gets blocked leading to pressure build-up. The fluid pressure build-up can be attributed to the deterioration of the optic nerve as well as genetic factors. The optic nerve of the eye is responsible for transmitting images to the brain.
Glaucoma, if not corrected or treated, can lead to severe damage as well as complete loss of vision. Many a time, glaucoma causes no pain or discomfort until the vision loss starts. Hence, it is essential to do regular check-ups to detect and treat eye diseases like glaucoma. Consult with Eye Mantra, to get in touch with the best Ophthalmologist across Delhi/ NCR providing the best Glaucoma consultation.
Glaucoma Causes
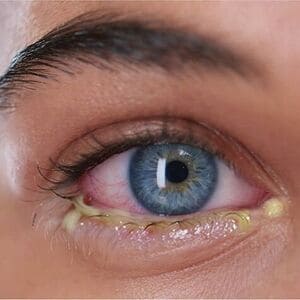
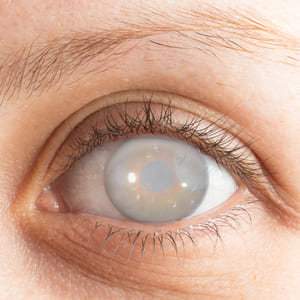
Glaucoma has been deemed by many doctors as the ‘silent thief of vision ‘ as it presents next to none or very few symptoms and many symptoms present themselves only after significant damage has been done to your vision. However, based on what type of glaucoma you might have there are certain symptoms that might be for early detection and management of glaucoma. They are:






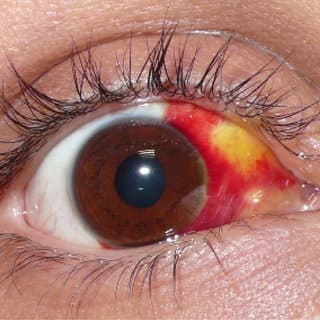
Glaucoma Surgery Risks

Glaucoma Surgery Cost
The complete cost of Glaucoma treatment depends upon the type of procedure or testing that you go through. The cost of treatment varies between Rs.3,500 to Rs.1.6L Per Eye. Below are estimated cost of some of the procedure, injections, testing and surgery involved in treatment of Glaucoma:
| Procedure | What It Does | Starting Price (Per Eye) | Suitable For |
|---|---|---|---|
| Peripheral Iridotomy (PI) | Creates a tiny laser opening to improve fluid flow | ₹3,500 | Early glaucoma / high eye pressure |
| Bleb Needling | Clears the blocked drainage area after previous surgery | ₹5,000 | Raised pressure after trabeculectomy |
| Bleb Revision | Repairs or improves a failed/weak bleb | ₹10,000 | When needling fails or pressure remains high |
| TRAB + MMC + Mannitol | Creates a new drainage channel to reduce eye pressure | ₹40,000 | Moderate–advanced glaucoma |
| TRAB + Phaco + IOL | Glaucoma surgery combined with cataract removal & IOL implant | ₹35,000 + cataract charges | Patients with both cataract & glaucoma |
| BANG (MIGS) | Minimally invasive procedure to improve drainage | ₹10,000 | Mild glaucoma wanting a safer option |
| AGV (Ahmed Glaucoma Valve) | Valve implant to control severe or uncontrolled pressure | ₹65,000 | Severe / medically uncontrolled glaucoma |
| iStent (MIGS) | Tiny implant to improve long-term fluid drainage | ₹1,60,000 | Mild–moderate glaucoma, often with cataract |
| Note: These are starting prices (per eye) and approximate. Final cost may vary after doctor evaluation and tests. | |||
Our Team

Cataract, Retina, Glaucoma, LASIK

Cataract, Squint, Oculoplastic

Cataract, Retina, Glaucoma

Cataract, Cornea
World-class Glaucoma center




Happy Glaucoma Patients

“I have been going to Dr. Shweta for the past few years for my glaucoma. I cannot praise her enough! Not only is she an excellent doctor, but she is also very kind and caring. She has always taken the time to answer all of my questions and make sure that I am comfortable with my treatment. I would highly recommend her to anyone looking for an outstanding ophthalmologist.!”
– Megha Kaushik
Frequently Asked Questions
Glaucoma is generally associated with a build-up of pressure inside the eye also called Intraocular Pressure (IOP), this happens when the fluid inside the eye aqueous humour stops draining from the eye.
Variants of open-angle glaucoma include Primary Open-Angle Glaucoma (POAG), Normal-Tension Glaucoma (NTG), Pigmentary Glaucoma, Pseudoexfoliation Glaucoma and Secondary Glaucoma.
If you are experiencing inflammation inside the eyes, halos in vision, light sensitivity etc then you should get tested for Glaucoma.
The cost of “Glaucoma testing” inclusive of “Fields +OCT + Pachy+ Gonio”, will be Rs.3,000. Other tests cost under 3000 Rs here at Eye Mantra.
No surgeries are free of risks. Some of the risks associated with Glaucoma Surgery are redness, pain, bleeding in the eye. You can also develop Cataracts later.
Blindness is one of the most adverse effects of glaucoma. And even though it is not necessary if you get diagnosed and treated at the right time then you can avoid loss of vision from Glaucoma.
There is no defined normal eye pressure as such but an average person has IOP between 12-22 mg Hg.
Although it is not recommended by optometrists marijuana is scientifically known to reduce eye pressure for a few hours. But since treating Glaucoma requires releasing pressure from the eye for the whole day, it is not feasible.
Even if one were to opt for this they’d have to consume copious amounts of it, which has considerable effects on the body.
There are multiple good Glaucoma surgeons in India. Eye Mantra has some of the top Glaucoma doctors / surgeons. Dr. Shweta Jain is one of the best Glaucoma surgeons in India. Dr. Shweta Jain has successfully performed more than 1000+ Glaucoma surgeries so far. The results from the Eye Mantra Glaucoma surgery program turns out to be better for many people. Post Glaucoma surgery, multiple patients experience improved appearance & depth perception
