Contents
Corneal Ulcer
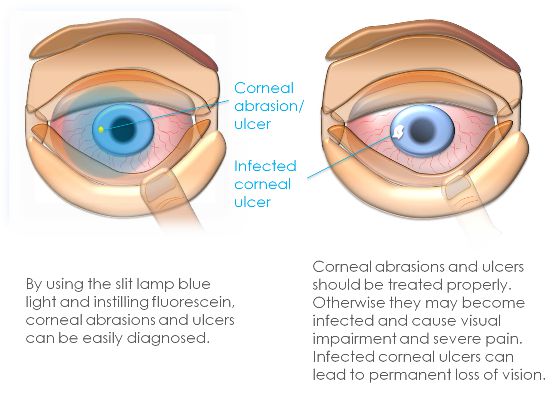
A corneal ulcer, also known as keratitis is an open sore in the cornea of your eyes. The cornea is the outermost layer of the eye that covers the pupil and iris. Our eyes work like a camera and the cornea is the window through which light passes inside the eye. The cornea is protected by a layer of tears, which defend the cornea from any foreign particles and infections.
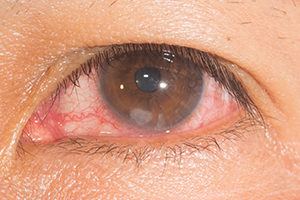
A corneal ulcer occurs because of, infection, fewer tears in the cornea, burns, extended use of contact lenses, dry eyes, or ocular herpes. The wound can be extremely painful with white or grey spots on the cornea, red-eye, swollen eyelids, excessive watering of the eye, redness, and blurred vision. Treatment of corneal ulcers and diseases depends on the cause. The corneal ulcer should be treated as soon as possible to prevent further damage to the cornea and vision change.
Symptoms of Corneal Ulcer
Symptoms vary from person to person, depending on causing factors. If the wound is caused by bacteria, it will be visible to the naked eye, within the white part of the cornea.
Not all corneal lesions appear without a microscope. However, especially if they are caused by the herpes simplex virus. Often, corneal ulcers are caused by symptoms such as:
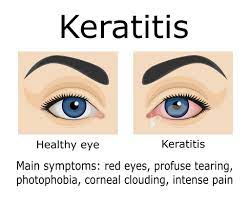
- The pain in the eyes (from being mild becomes severe, then it becomes more intense).
- Sclera turns red and forms conjunctiva (white part of the eye with its clear cover).
- Photophobia (sensitivity to light)
- Blurry vision
- Swollen eyelids
- Tears
- A feeling of a foreign particle in the eye
Causes of Corneal Ulcers
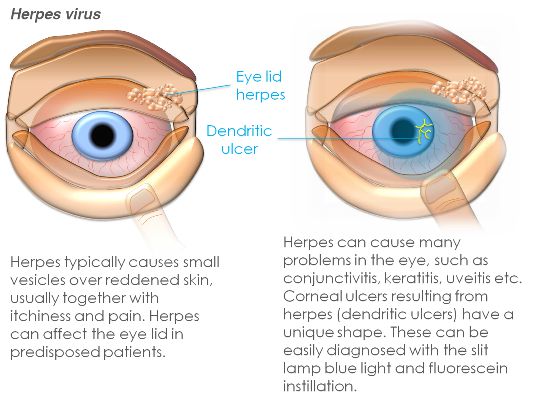
In severe cases, it is caused by germs that enter through previous injuries or scratches in the cornea. Bacteria can also be viral, fungal, or they can be infectious. If the sore is caused by the herpes simplex virus it is called a dendritic ulcer, and it will not be visible to the eyes.
The herpes simplex virus can be a common infection of the virus that most people contract in childhood. Symptoms of the virus often include cold sores, pharyngitis, and swollen glands. It is not uncommon for the virus to spread to other parts of the body, but this will only happen if you touch the infected area and then touch your eye.
Corneal ulcers are more common in those who wear contact lenses, perhaps as a result of rubbing or contaminated contact lenses on the eyes. In the event of a lot of scratching, a portion of the skin may become weak and broken, causing bacteria to invade and begin to reproduce and spread.
Lens carriers who do not keep proper hygiene also increase their chances of developing corneal ulcers. For example, wearing soft lenses while sleeping, or being unhygienic when removing or repairing lenses increases the exposure to germs that can lead to infection.
Studies have shown that wearing night-contact lenses is a major cause of infection. Acanthamoeba (acanthamoeba keratitis) is a common eye infection. Contact lens wearers who fail to remove their lenses before swimming can get a parasitic eye infection.
Additional causes of corneal ulcers may include:
- Allergies
- Corneal abrasions
- Viral, fungal infections
- Dry eyes
- Disorders of the immune system
- Parasitic infections
- Inflammatory diseases such as multiple sclerosis and psoriasis.
Risk Factors For Corneal Ulcer
If you have had a corneal injury in the past, you are considered at risk for long-term damage to the cornea and you will experience significant changes in your vision over the long term. Additional components that increase the risk of ulcers include:
- Using contact lenses, especially soft lenses, while sleeping
- Having dry eyes
- Recent infection or injury
- Severe allergic reactions
- Eyelids that do not close completely
- Failure to wear eye protection during sports
- A weakened system, such as often caused by HIV
- Work or hobbies that use tools that produce dust, such as farming or construction work.
Corneal Ulcers Complications
Serious complications from corneal ulcers occur because the wound is not treated properly. Often, treatment can prevent problems such as:
- Loss of vision
- Fracture of the cornea
- Loss of the affected eye due to cataract or glaucoma
- Dispersal of infections in other parts of the eye and body
- Severe pain
- Any change in vision
- Exposure to the foreign particle within the eye
- Exposure to chemicals or flying particles
Corneal ulcers should not be ignored. If you experience symptoms of corneal ulcer, you need to seek medical help immediately.
Prevention of Corneal Ulcer
If you have an eye infection or feeling some kind of discomfort in your eyes, you need to get immediate medical attention from an ophthalmologist or an optometrist. Early treatment can prevent the wound from growing. Contact lens wearers should wash their hands before handling contact lenses to prevent the transmission of germs and foreign substances. Stop wearing contact lenses while sleeping. Speak to your eye care professional about the other preventive measures you need to take during your normal daily activities, according to your routine.
Treatment of Corneal Ulcers
To treat corneal ulcers, a doctor will first find the seriousness of the ulcer. Treatment should not be delayed as the corneal lesions grow. If the cause is unknown, antibiotics are prescribed to fight any potential bacterial infection.
Antibiotics are usually administered within the form of eye drops, sometimes in combination for an hour. In some cases, corticosteroid eye drops are prescribed to measure inflammation.
If the corneal lesion is severe, corneal implants (keratoplasty) may be required. In this procedure, the diseased or injured cornea is removed. The new cornea is then attached to the care of the small muscles (stitches). Joints are removed after the end of healing, usually a few weeks after surgery. Most people see an improvement in their vision a few days after surgery. In some cases, hospital stays are as long as two days.
Your optometrist may also recommend to:
- Wear safety goggles
- Take painkillers
- Avoid eye makeup
- Avoid sharing cosmetics, towels, or eye drops with others
- Stop wearing contact lenses during treatment
- Stop wearing contact lenses while sleeping
- Wear an eyebrow patch to avoid symptoms such as sensitivity to light
- When performing a keratoplasty, do not let water get into your eye
Follow-up visits with your optometrist are often recommended, no matter how severe the wound may be.
For any eye-associated issue, visit our hospital in Delhi now or visit our website- www.eyemantra.in Call +91-9711115191 or mail us at [email protected] to book an appointment with us.
Our team of great and experienced ophthalmologists will always suggest the best options for your eyes.